My mom had driven all the way from my hometown in Arizona to be present at the birth of her first grandchild and to help me settle in to motherhood. We were hanging out at her AirBnB, enjoying the air conditioning and each other’s company, when it happened. It was a hot summer day, and at 39 weeks pregnant, I was draped across the length of her white couch in an effort to get as much cool air on my body as possible. We were mid-conversation when I felt a warm, wet release in my vagina. I shot off the couch like a rocket.
“I think my water just broke,” I said.
Mom looked at me with big eyes and an excited smile. “Are you sure?”
I ran to the bathroom and sat on the toilet. Fluid dripped between my thighs and a little red-brown mass plopped down into the water.
“Yeah,” I said, “I’m pretty sure!”
I was laughing now. Laughing with joy and shock and disbelief. I hadn’t expected my water to break before I started having contractions. This is called prelabor rupture of membranes, and it only happens in 10-20% of births, depending on the source. Just that morning, I had seen my OB for my 39 week appointment. She had checked my cervix and reported that my dilation was “one and a wiggle,” nothing to write home about. We scheduled an induction for 41 weeks. She told me I would get a call about scheduling a modified biophysical profile test for my baby on my due date. And here I was, mere hours later, clutching a towel between my legs and calling the after-hours nursing hotline.
I drove home to collect my husband and our go-bags, and before we knew it we were in our private room at the hospital. It was about 6:00 pm. The labor and delivery nurse was reviewing my medical history, asking me intake questions, and reviewing my birth plan. She noted that I was hoping for a non-medicated, low-intervention, spontaneous vaginal delivery, aka “natural” birth. Specifically, I wanted to avoid using an epidural so that I could be up out of bed for as long as possible. Because my water had already broken and my cervix remained barely dilated, my medical team suggested I take a cervical ripening agent called Cytotec. I politely declined, opting to wait and let my body take control, as I had planned to do.
I had been preparing to deliver my baby with as few medical interventions as possible since my second trimester. Affirmations, visualizations, meditation, aromatherapy, and birth prep exercises had been part of my routine for many months. In my hospital room, I taped up photographs of my mother, my sister, my grandmothers, and my great grandmothers to invoke their strength and courage. I cued up my birth playlist and got out the diffuser. I sat down on the birth ball and began moving my pelvis in smooth, clockwise circles. Later, I walked the halls holding hands with my husband. Soon I was doing squats in the hallway, lunges across my room, and what felt like endless laps of the unit. I did everything I had prepared to do, and yet, the contractions refused to come.
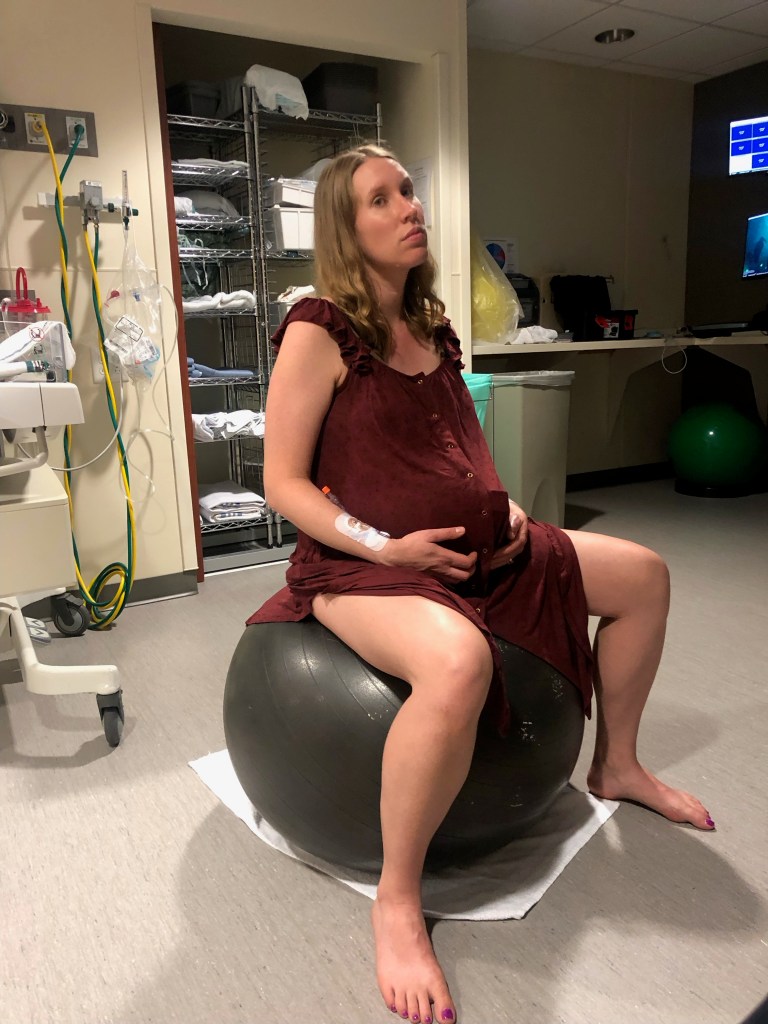
I decided to take the Cytotec and continued moving and breathing. Eventually, I would take three rounds of this medication with very little progress to show for it. I also used a breast pump twice in an effort to use nipple stimulation to increase oxytocin release. At this point, I was having contractions frequently, but they were irregular. They felt like a very strong menstrual cramp. Each contraction was enough to slow my steps and demand my attention, but my cervix ceded only another centimeter or two. We were deep into the nightshift now, and I felt stuck, exhausted, and frustrated. Still, I was determined to stay the course. I kept walking. I ate. I rocked on the ball. Meanwhile, my husband and my mother took turns napping. One of them stayed by my side while the other slept in anticipation of what was to come.
Sometime in the wee hours of the morning, the OB approached me to talk about next steps. She found me looking out the window at the coming dawn, my husband cradling me as I sobbed tears of frustration and fatigue. She recommended that I start Pitocin, a synthetic form of oxytocin, to induce labor. I agreed, although I was not happy with the decision. Back in my room, my mother comforted me, holding me, braiding my hair.
“I didn’t expect my body to need so much help,” I said tearfully.
“It’s ok, there’s nothing wrong with needing help,” she said, and held me closer.
At 7:00 am, about 14 hours after I my water broke, the nurses changed over and we met Elsa.* Meeting this nurse was a turning point in my experience. Elsa radiated a sort of joyful confidence. She was like sun breaking through my clouds. And she was exactly the person I needed at that moment.
Elsa was an experienced labor and delivery nurse, as well as a birth doula. She was also a fierce advocate for her patients. Because of Elsa, we discovered that part of my lack of progress was due to the presence of something called a forebag. I had never heard of this phenomenon, and it is difficult to find accessible information about it on the internet (if you are a L&D nurse or birth provider, please share your knowledge in the comments!). As I understand it, sometimes when a person’s water breaks the baby descends in the pelvis and makes a plug of fluid just above the cervix, sort of like creating a new, smaller bag of water. If this forebag is not broken, either naturally or by a provider, it can delay labor. When Elsa discovered the forebag during a cervical check, she immediately notified the resident. They appeared not long after and broke the forebag with something that looked like a crochet hook.
My labor started progressing more quickly then, and the contractions were getting stronger and more difficult to manage. After Elsa started me on a Pitocin drip through my IV, she led me through a series of movements and hands-on adjustments to help my baby move into a more optimal position for birth. The technique she used is called Spinning Babies. I remember how supported I felt by Elsa as we moved together. She literally held me as each contraction washed over my body like a wave. Despite the increasing intensity of each contraction, I managed to smile and even laugh as we spoke. She filled the room with positivity, talking about her little girl and her cat, and she continued to uplift me with words of encouragement and validation. Soon, she was instructing my husband in how to perform a specific technique she was using and directing my mom to fill the large tub in the bathroom. As she helped us navigate my birth process, she empowered each of us—she empowered my mom and my husband to be helpful and supportive birth partners, and she empowered me to stay committed to my vision of a low-intervention birth without an epidural. Every time my proverbial fire sputtered, she was there to rekindle it.
The next thing I remember is submerging myself in the tub. The warm water rippled around me and I felt a sense of buoyancy and ease. My husband sat in front of the tub with a cool wash cloth and a bowl of ice chips. Between contractions, which were coming rapidly and painfully, I rested my head on the edge of the tub and sucked on ice.
“Keep your voice deep and low,” Elsa said as I cried out in a high-pitched, sharp tone during the next contraction. I did as she said and felt my body soften. As each contraction moved through my body, I moaned, “huhing” and “hahing” in a low voice with Elsa’s coaching.
Then, the transition phase hit. Transition is the final, but usually most intense phase of labor. In this stage, the cervix dilates from 8 to 10 centimeters. The next contraction came quickly and with a ferocity I could have never prepared for. As it gripped my body, I had the thought that I could not go on, that surely this would kill me. I called out for my husband, who held my hand and said, “I’m here.” Then I called out for Elsa. As she met my gaze she said with utter confidence and determination, “You can do this.” I believed her.
Soon my mother was helping me step out of the water and leading me back to the bed to begin pushing. I started out on my hands and knees, but I moved to lying on my side after one or two pushes. In this side-lying position, Elsa held up my top leg and guided me through each push while my husband sat at the head of the bed and held my hand and stroked my hair. I pushed for 34 minutes. The OB sat at the foot of the bed on a stool the entire time, calmly awaiting my baby and gently encouraging me. As a searing, burning pain took over my body she looked at me and said, “This is the ring of fire, Savannah, the ring of fire.” My baby was crowning, and somehow, knowing that it was supposed to be excruciating made it more tolerable.
On the last push, everyone in the room was cheering me on and telling me just how close I was to meeting my baby. I remember thinking in that moment that I just could not push anymore; this would have to be the last one. I willed myself to push harder and longer than I thought I could. Suddenly, I felt my baby emerge. I saw the OB lift my baby up and unravel the umbilical cord that wrapped itself around her torso like a sash. “It’s a girl!” my mother exclaimed. And then, finally, the OB placed my baby girl on my chest.
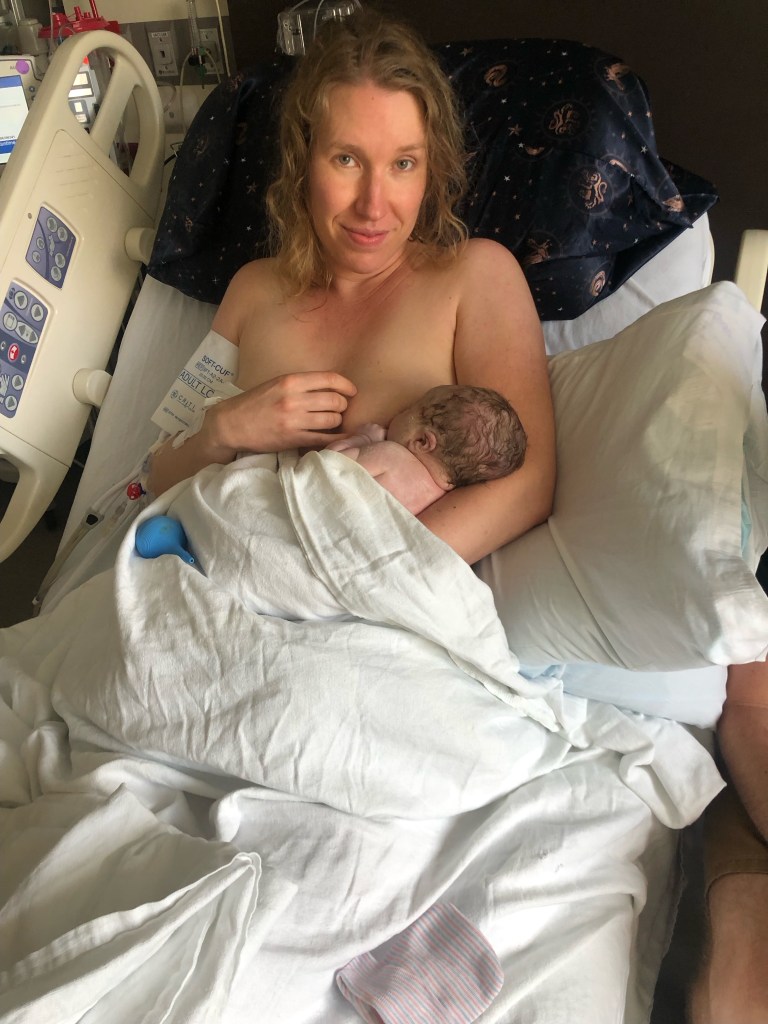
Relief, astonishment, gratitude, bliss, awe. I felt it all, all at once. And more than anything else, I felt my heart, my capacity to love, expand exponentially. I never knew I could love someone so deeply and so fiercely. Yet here was this precious, squished, purple little creature, making me love more than I thought possible. I held her close as she started searching for my breast. She found it and latched on, with a little help, of course. During all of this, my feet were in stirrups while the OB stitched up my tear. I ended up with a 2nd degree tear, which means some of my pelvic floor muscles tore during birth. I had expected to tear a little bit, so I was not surprised to hear I needed a few stitches.
After the OB finished the repair, my husband and I were left alone for about two hours to bask in the love and light of our little girl without any interruption. I couldn’t take my eyes off of her. I felt a sense of wholeness as I held her, like I now had everything I needed in my life. Everything else suddenly seemed so small. And I imagine I’ll always feel that way now that I’m a mother. For me, having a child has taught me what is truly important in life. Things I used to worry about are suddenly irrelevant. Loving her, keeping her safe, and providing for her is all that matters now. My heart is forever bound to hers. And because of her, my heart will always be full.
***
Even now, just five months later, the details of my daughter’s birth are getting hazy. I find that what remains just as sharp are the feelings. The overwhelming love I felt as I held my little girl for the first time. The deep gratitude I felt for my husband and my mother, and the pride I took in watching my husband handle the entire experience with ease and courage. The immeasurable appreciation and love for Elsa, the doula nurse who guided my baby into this world and guided me into motherhood.
No one should have to enter motherhood alone. I am fortunate to have a true village of family and friends who supported me as I began this new chapter of my life. I am so grateful to my husband, my mother, my friends, my amazing postpartum doula, Kathleen, and my medical team at Mercy St. Louis, all of whom uplifted me and guided me in their own essential ways.
Birth changed me. I imagine it changes every person who embarks upon this incredible journey. Luckily, I had numerous people ready to stand at my side as I transitioned into motherhood. If you would like to support other new moms as they prepare for and recover from birth, I encourage you to donate to the Rhea Community Fund. Donations to this fund are used to provide birth prep and postpartum recovery services to moms who need financial aid, helping them to get the critical pelvic health care they need, no matter their financial situation. Click here to make your donation today.
*This nurse’s name has been changed to protect her privacy.

